Signs Your Pelvic Floor May Be Weak Postpartum
What are the signs your pelvic floor may be weak and what does this mean after having a baby?
Bringing a baby into the world is one of the most physically and emotionally transformative experiences a woman can go through. The exhausting sleep deprivation, round-the-clock feeds, and emotional ups and downs, it’s easy to overlook your own recovery, and especially the health of your pelvic floor. Yet for many women, this group of muscles becomes a source of unexpected symptoms and quiet concern in the months following childbirth.
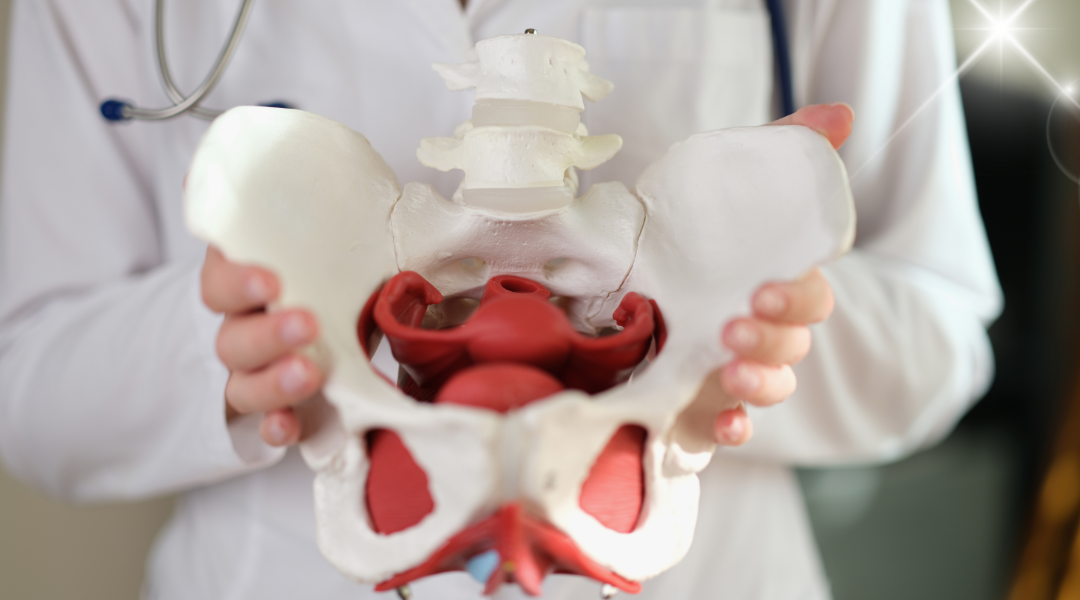
What is the pelvic floor?
Your pelvic floor underwent significant changes during pregnancy and birth. These muscles, which normally work like a supportive hammock at the base of your pelvis, had to stretch and adapt to accommodate your growing baby and the birthing process. Understanding how childbirth specifically impacts these muscles can help you recognise when they need extra support during your recovery.
But life isn’t ideal, and more often than not, doing kegel exercises goes by the wayside (particularly when a problem isn’t physically evident!)
The common signs your pelvic floor is weak
1. Leaking when you laugh, sneeze or lift your baby
Perhaps the most talked-about (and simultaneously most quietly endured) symptom of pelvic floor weakness is stress urinary incontinence. This happens when your pelvic floor muscles, which were stretched during pregnancy and delivery, can no longer provide adequate support during everyday activities like sneezing, laughing, or lifting your growing baby.
During childbirth, the muscles supporting your bladder may have been stretched or strained beyond their normal capacity. The weight of pregnancy combined with the physical demands of delivery can affect how well these muscles respond when you need them most. If these muscles can’t contract properly, urine may escape even with minor effort or strain. Some women experience just a few drops during a sneeze, while others may feel the need to wear a liner every day to feel secure.
This experience can be really emotionally distressing. It doesn’t seem fair that we are experiencing incontinence in our 20’s or 30’s - something you’d normally associate with growing old. It may cause new mums to avoid exercise, limit social outings, or feel disconnected from their own bodies. However, it’s important to understand that while common, incontinence is not something you simply have to live with. Pelvic floor therapy and guided rehabilitation can significantly improve or even fully resolve leakage.
2. A heavy or dragging feeling in your pelvic area
Another lesser-known but incredibly common symptom of pelvic floor weakness is a sensation of heaviness or dragging in the vaginal or pelvic area. Some women describe it as feeling like something is “falling out” of their body, or like there’s a tampon inserted incorrectly. This sensation may worsen throughout the day, particularly after standing, walking, or lifting.
This heaviness often develops after childbirth when the support structures have been stretched during delivery. Your uterus, which expanded significantly during pregnancy, may need time to return to its pre-pregnancy position and support level. Pregnancy, labour, and delivery are all major risk factors for prolapse, especially if you had a long pushing stage, delivered a large baby, or required an assisted birth using forceps or vacuum.
While the word “prolapse” may sound alarming, many mild cases can be managed extremely effectively with conservative treatment. Pelvic floor physiotherapy, postural guidance, and lifestyle modifications (such as avoiding heavy lifting and managing constipation) can help alleviate symptoms and prevent progression. With early intervention, surgery is rarely necessary.
3. Difficulty controlling wind or bowel movements
Changes in bowel control are perhaps the most embarrassing postpartum symptoms that new mothers face, yet they're more common than you might think after delivery. After giving birth, especially if you experienced tearing near the back of the perineum (third- or fourth-degree tears), you may notice changes in how well you can control wind or bowel movements. Some women experience urgency, where they feel a sudden and strong need to empty their bowels, while others might struggle with holding in gas or suffer from minor faecal leakage.
Bowel incontinence can arise when the anal sphincter or surrounding pelvic floor muscles are damaged or weakened during childbirth. Even without a diagnosed tear, nerve and tissue trauma from prolonged labour can affect the coordination and control of the muscles responsible for continence.
Understandably, these symptoms can be deeply upsetting and impact your sense of autonomy and dignity. But they are not uncommon, and most importantly they are treatable. A pelvic health physiotherapist can provide tailored guidance, including techniques to improve muscle tone, restore sensation, and regain control.
4. Pain or discomfort during sex
For many women, the thought of intercourse after childbirth is accompanied by uncertainty, fear, or even dread. While some level of discomfort is expected in the early weeks postpartum especially after a vaginal delivery, tear, or episiotomy, persistent pain during sex can be a sign of underlying pelvic floor dysfunction, and it is important to get it checked out.
Some women experience tightness, burning, or a feeling of resistance, particularly at the vaginal opening. Others may feel that sex simply isn’t pleasurable anymore due to a loss of sensation or confidence in their body. This can stem from scar tissue, hormonal changes (especially if breastfeeding), or a pelvic floor that is either too weak to support sexual function or too tense from trauma and protective muscle guarding.
The emotional impact of painful sex is significant. It can create a sense of disconnect in relationships, lower self-esteem, and add to the emotional load of motherhood. But again, help exists, with proper rehabilitation sometimes including gentle internal work, scar massage, or topical estrogen treatments many women regain comfort, function, and a renewed sense of intimacy.
5. Feeling the urge to wee all the time?
If you feel like you are always running for the toilet, or still feel the urge when you have emptied your bladder, then you may be experiencing urge incontinence. Frequent urination or a constant urge to wee, even shortly after you've just been, is yet another indicator that the pelvic floor isn’t functioning optimally. Urge incontinence is an extremely delipidating condition effecting men and women, but particularly if you are new mum, night wees is the last thing you need!
The condition can manifest as an overactive bladder, where the signals between the brain and bladder become hypersensitive, or where pelvic floor weakness causes poor support to the bladder and urethra. Sometimes, trauma during birth can cause the bladder to shift position slightly, affecting how well it empties and leading to that frustrating sense of urgency.
These symptoms can be especially challenging with a new baby, when sleep is already broken and outings require strategic planning, but with guidance, it’s possible to retrain the bladder, strengthen supporting muscles, and regain a more predictable and comfortable urinary rhythm.
Your healing takes time
Recovering from birth is not a six-week job, despite what the traditional check-up schedule might suggest. Your pelvic floor, like any group of muscles recovering from strain or injury, needs time, attention, and the right kind of rehabilitation. Every woman’s journey is different, and it may not end up being what you thought it would be. We can’t predict what will actually happen during your birthing experience, but also your genetics, lifestyle, physical and mental health and the human support systems you have in place to help you, all play a role.
What are your postpartum recovery options?The encouraging news is that postpartum pelvic floor issues often respond well to targeted rehabilitation. Many new mothers benefit from seeing a women's health physiotherapist who specialises in postpartum recovery. They can assess how childbirth specifically affected your muscles and create a personalised recovery plan that fits around your new baby's schedule.
The role of advanced treatments like Emsella in postpartum recovery
For new mothers dealing with ongoing pelvic floor challenges, sometimes traditional kegel exercises aren't enough - especially when you're exhausted from sleepless nights and focused on caring for your baby. At Springwell Clinic, many postpartum women have found significant relief through specialised pelvic floor rehabilitation.
The clinic's Emsella treatment offers intensive muscle strengthening that's particularly valuable during postpartum recovery. This non-invasive chair-based treatment delivers deep pelvic floor contractions that would be impossible to achieve through voluntary exercises alone - especially beneficial when you're dealing with weakened muscles from pregnancy and childbirth.
The treatment works by targeting the entire pelvic floor network, helping to restore the comprehensive support these muscles provided before pregnancy. Each session strengthens not just the primary pelvic floor muscles, but the surrounding support structures that were affected during your birthing experience.
For busy mothers, the convenience factor is crucial - sessions require no preparation, you remain fully clothed, and there's no recovery time needed. You can literally fit treatment into your schedule between baby's naps or during childcare.
Rajinder experienced persistent stress urinary incontinence following the births of her three children. Like many mothers, traditional exercises weren't providing the results she needed for her active lifestyle and confidence. Watch Rajinder's postpartum recovery story here:
[embed]https://www.youtube.com/watch?v=hyIn44j2T_Q[/embed]
If you recognise yourself in any of the signs described above, please don’t suffer in silence or dismiss them as something you “just have to live with.” Talk to your GP or a pelvic health specialist, or if you would like to learn a little more about Emsella and your suitability for treatment, get in touch with us on 01628 308060 or email hello@springwellclinic.co.uk.
You can also book a consultation online on our booking system.
We will be releasing further blogs focussing on your Pelvic Floor over coming weeks, so keep up to date in our News section!